On June 1, 2018, New Jersey Governor Phil Murphy signed the Out-of-Network Consumer Protection, Transparency, Cost Containment and Accountability Act (the NJ Surprise Bill Act) into law. This legislation, in part, prohibits the practice of balance billing patients and increases transparency in medical billing.
The purpose of the law is to protect patients from unexpected or “surprise” medical bills that sometimes arise when a patient unknowingly receives treatment from an out-of-network provider and is then billed for the difference between the provider’s billed charges and reimbursement received from payors for services performed in emergency room/urgent and/or inadvertent care settings.
Generally, the NJ Surprise Bill Act applies to fully insured plans, the State Health Benefit plans, and self-funded plans that have opted into being governed by the NJ Surprise Bill Act. Beginning January 1, 2022, the new Federal No Surprises Act will govern self-funded surprise bill claims that have not opted into NJ law and those fully insured claims for services not covered by the NJ Surprise Bill Act, such as post-stabilization care.
As of January 28, 2021, 137 self-funded plans opted into the arbitration process, including:
- NJ Manufacturers
- Kearny Bank
- CentraState Healthcare System
- Redfin Corporation
- Roosevelt Paper Company
For the complete list, check out NJ DOBI‘s site.
Key Requirements
The NJ Surprise Bill Act outlines new requirements that affect health care professionals in the following areas:
- Disclosure and notification: Health care facilities and providers must disclose information regarding network status, medical codes, and estimated fees to patients before scheduling nonemergency procedures or elective services.
- Balance billing prohibition: Facilities and providers may no longer bill patients for costs exceeding their in-network deductible, copayment, or coinsurance when billing for medically necessary urgent or emergency services or inadvertent OON services.
- Mandatory assignment of benefits: Whenever patients receive inadvertent emergency or OON services, it automatically results in the assigning of the benefits under the patient’s carrier to the OON provider with no further action required by the patient.
- Arbitration process: When carriers and providers disagree on an emergency or urgent medically necessary service or inadvertent OON service and the disputed amount exceeds $1,000, either party may initiate a binding arbitration process to resolve the issue if negotiations fail to resolve the payment dispute.
- Prohibition of cost-sharing waiver: No OON providers may waive or offer to waive all or a portion of a patient’s deductible, coinsurance, or copayment to induce them to choose medical care from that provider. The prohibition does not apply to activities falling under federal safe harbors, which are legal provisions designed to provide protection from liability when meeting specific conditions.
How Is the NJ Law Impacting OON Providers?
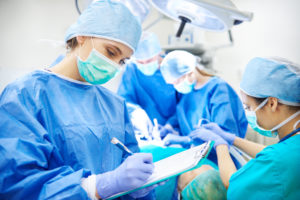
The NJ Surprise Bill Act has changed the landscape for OON surgeons and other medical practitioners regarding their billing practices and procedures. They need to be more knowledgeable and adept at identifying claims subject to the State surprise billing law and must comply with the time-sensitive requirements for handling these claims.
The time frames for negotiating and arbitrating surprise bill claims according to the statute specify that insurance carriers have 20 days to either pay the bill or notify the provider that the billed amount is excessive. The provider then has 30 days to dispute the proposed payment and negotiate a final reimbursement amount with the carrier.
In the event the payor and the provider are unable to resolve the payment amount, either party may initiate the “baseball-style” binding arbitration whereby the arbitrator must select one of the two final amounts submitted within 30 days.
Contact Us to Learn More About the NJ Surprise Bill Law
Cohen Howard has been helping surgeons navigate the new surprise medical bill law since it was enacted August 30, 2018. We remain committed to negotiating and arbitrating these claims to maximize your reimbursements. The Federal No Surprises Act (NSA) takes effect on or after January 1, 2022 and will be the default law to prohibit the practice of balance billing patients in certain instances. Otherwise, State-specific laws that have a methodology for handling disputes between payors and providers will preempt the NSA.
The determination will depend on a number of factors, including the type of services rendered and the type of policy for which a given claim is covered. Timely filing will be a much bigger factor, as under the NSA the negotiation and arbitration processes are well defined and, in many cases, much narrower than State law time requirements.
Do you have questions about the Surprise Billing Laws, the No Surprises Act, or any other aspects of the Surprise Bill Law in NJ? Cohen Howard has answers. Our legal services can increase revenues for OON providers when dealing with insurance companies. Contact our firm today at 732-747-5202 for a free consultation or any additional information.